Le Questionnaire médical (à imprimer en recto/verso uniquement 1 feuille ou à remplir sur place) qui est rempli pour le don du sang est aussi valable pour le don de plaquettes.
Lire également le Formulaire d'information des prescriptions Transfusion CRS Suisse.
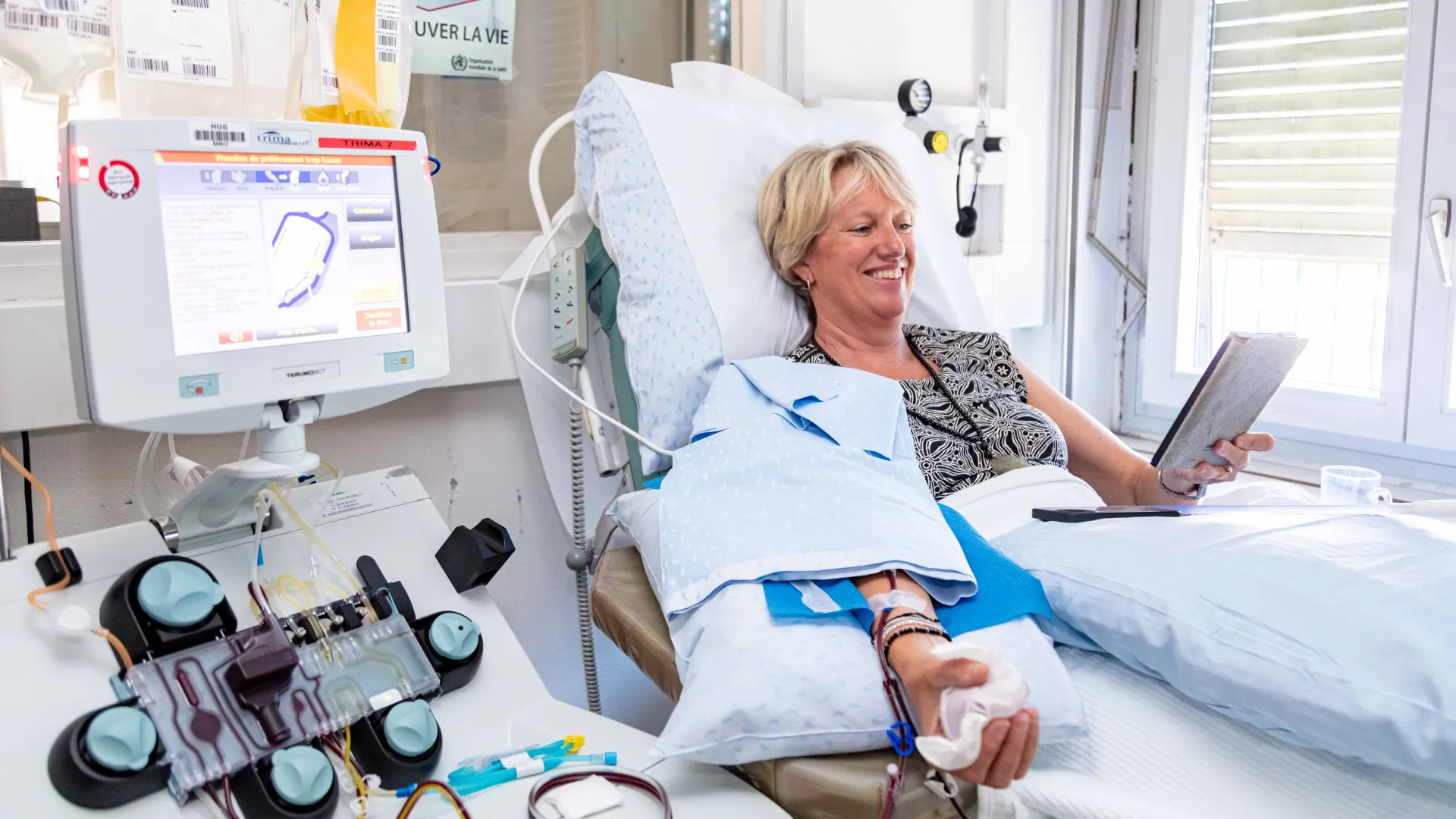
Peut donner ses plaquettes toute personne
- en bonne santé générale, pesant au minimum 50 kg
- ayant déjà donné au moins une fois son sang (taux de plaquettes minimum entre 250 000 et 300 000)
- et âgée de 18 à 60 ans. Les donneurs réguliers peuvent faire des dons jusqu’à 75 ans.
Certaines circonstances contre-indiquent le don de plaquettes. En particulier, une intervention dentaire (y compris un détartrage) dans les 72 heures précédant un don de plaquettes ou une température supérieure à 38°C au cours des 15 jours précédents.
Il faut également éviter la prise de certains médicaments qui inhibent la fonction plaquettaire et rendent ainsi les plaquettes inutiles pour la transfusion. Il s’agit de l’Aspirine sous toutes ses formes et des anti-inflammatoires non stéroïdiens tels que le Ponstan, le Felden, le Tilcotil, le Brufen, l’Indocid et le Voltarène, pour n’en citer que quelques-uns. En revanche, le Panadol (paracétamol) peut être pris à condition qu’il ne soit pas associé à un des médicaments ci-dessus.
Les tests habituels de qualification au don du sang sont pratiqués sur le don de plaquettes, et comprennent le dépistage de la syphilis, des hépatites B et C, et de l’agent du sida.