- Homepage
- The Centre
- Research & innovation
- Virtual Medicine Center
- Outpatient clinic for brain and mental health
Neurocentre
Neurocentre
Neurocentre
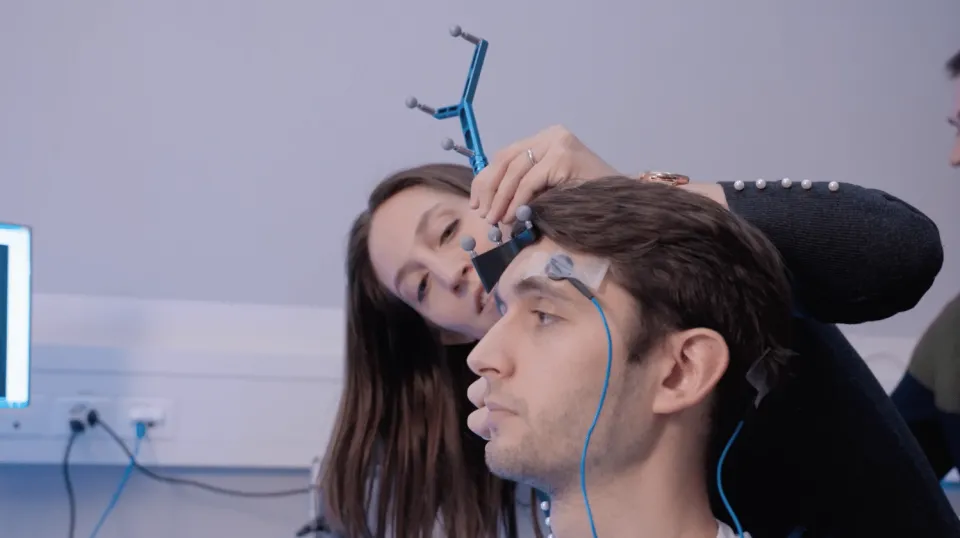
The research group is led by Elena Beanato, who holds a PhD in translational neuroscience. Her team at HUG is exploring a new non-invasive approach for restoring cognitive function – and especially spatial orientation capabilities – after a head trauma and in cases of epilepsy. Their approach uses electric fields to carry out transcranial deep brain stimulation, eliminating the need for invasive surgery.
People’s ability to orient themselves in their surroundings – an essential function of the human brain – can be temporarily or permanently altered by even a mild traumatic brain injury (like a concussion) or some forms of epilepsy. Around 80% of traumatic brain injuries can be classified as mild to moderate and, of these, nearly 15% result in a disorder that continues more than six months after the trauma. This disorder includes impaired spatial memory, an inability to situate oneself and disorientation. “Even simple tasks like getting your bearings in a city, finding your way and remembering familiar routes can become a real challenge,” says Elena Beanato, a project manager at the HUG Outpatient Clinic for Brain and Mental Health. For now, few options are available for treating this condition.
Beanato’s cross-disciplinary research group is working to change that by developing an innovative method for deep brain stimulation without invasive surgery. The team has designed a procedure that uses temporal interference to stimulate areas deep inside the brain. In their method, two high-frequency electric fields are applied to a patient’s scalp. “The two fields intersect deep within the patient’s brain and produce a modulation that can influence neural activity in a targeted way – particularly in the hippocampus, which is a key region for memory and spatial orientation,” says Elena Beanato. In this project selected for the 2026 Leenaards Science Prize, she is working with Prof. Friedhelm Christoph Hummel, head of EPFL’s Hummel Lab and associate professor at the UNIGE Faculty of Medicine, and Prof. Pierre Mégevand, a neurologist at HUG and researcher at the Human Neuron Lab at the UNIGE Faculty of Medicine.
Potential applications for other neurodegenerative diseases like Alzheimer’sTo better understand how their new method affects cognitive function, the research team is working with epilepsy patients who received intracranial electrode implants as part of their treatment. “These sensors give us a unique window into how the human brain works,” says Prof. Mégevand. “We gain important insight into how the electric fields affect patients’ neural activity.” In the second phase of the research, the team is testing their method on patients who have suffered brain trauma. These patients are placed in an immersive virtual reality environment, and scientists measure their ability to orient themselves and move around, both before and after receiving the stimulation. “Our initial tests seem to confirm that the electric-field stimulation improves patients’ spatial orientation capabilities,” says Prof. Hummel. “We hope to eventually develop rehabilitation strategies as well as new therapeutic approaches.”
“Our research brings together neuroscience, engineering and clinical practice to develop a new generation of non-invasive treatments for cognitive disorders,” the project team explains. If further tests confirm the effectiveness of the team’s method, it could give doctors a safer, less complicated alternative to the surgical procedures currently being used. And it could open up new research avenues for other cognitive disturbances and certain neurodegenerative diseases such as Alzheimer’s by directly targeting the associated neural networks.
