Medical activities of the Digestive Surgery Division
 Digestive surgery, also named visceral or abdominal surgery, is the surgery of digestive organs, such as:
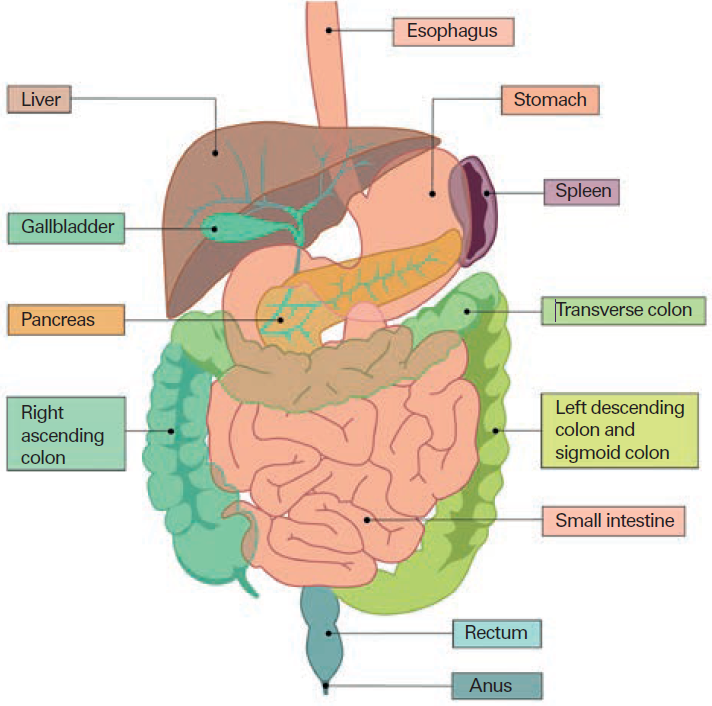
Digestive surgery, also named visceral or abdominal surgery, is the surgery of digestive organs, such as:
- the esophagus
- the stomach
- the small intestine
- the colon (large intestine)
- the rectum
- the anus
- the liver
- the gallbladder
- the pancreas
- diseases of the abdominal wall, such as hernias and incisional hernias (hernias on scars)
- implantable venous access devices (for long-term administration of products into the venous system).
The Division of Digestive Surgery offers multidisciplinary care at university level
The Division of Digestive Surgery is recognized as a leading center in terms of surgical expertise, and offers the highest level of care, coordinated in a multidisciplinary manner. In order to ensure quality of care and safety, the team of the division works closely with specialists in gastroenterology, transplantation, digestive oncology, anesthesia as well as diagnostic and interventional radiology.
The Division of Digestive Surgery brings the latest technological and scientific innovations at the service of patients
Minimally invasive surgery by laparoscopy
Contenu
Laparoscopy is a surgical technique that involves performing a diagnostic and/or therapeutic intervention through small incisions on the abdomen (keyhole technique). An incision is usually made at the level of the umbilicus to introduce a camera into the abdomen and to insufflate a gas (CO2), to dilate the abdominal cavity and obtain a space sufficient for good visualization. The camera is equipped with a light source and a sensor that transmits the images to screens for the surgical team. Other small incisions are made to introduce the surgical instruments, which are located at the end of long rods handled by the surgeons.
This technique makes it possible to avoid open surgery of the abdomen, to have reduced post-operative pain and to have a shorter hospital stay. Laparoscopy is performed when medically possible and indicated, for all types of surgery, whether of the abdominal wall (hernias), stomach, small intestine, colon, rectum, liver, pancreas or spleen.
Minimally invasive surgery by laparoscopy
Contenu
Laparoscopy is a surgical technique that involves performing a diagnostic and/or therapeutic intervention through small incisions on the abdomen (keyhole technique). An incision is usually made at the level of the umbilicus to introduce a camera into the abdomen and to insufflate a gas (CO2), to dilate the abdominal cavity and obtain a space sufficient for good visualization. The camera is equipped with a light source and a sensor that transmits the images to screens for the surgical team. Other small incisions are made to introduce the surgical instruments, which are located at the end of long rods handled by the surgeons.
This technique makes it possible to avoid open surgery of the abdomen, to have reduced post-operative pain and to have a shorter hospital stay. Laparoscopy is performed when medically possible and indicated, for all types of surgery, whether of the abdominal wall (hernias), stomach, small intestine, colon, rectum, liver, pancreas or spleen.
Minimally invasive robotic surgery
Contenu
Robotic surgery is a surgical technique consisting of performing a diagnostic and/or therapeutic intervention through small incisions on the abdomen, then setting up a surgical robot through which the surgeon will operate from a remote-control console. An incision is usually made at the level of the umbilicus to introduce a camera into the abdomen and to insufflate a gas (CO2) to dilate the abdominal cavity and obtain a space sufficient for good visualization. The camera is equipped with a light source and a sensor that transmits the images to the main surgeon's remote console and to screens for the surgical team. Further small incisions are made to introduce the surgical instruments which are controlled by the arms of the surgical robot. The surgeon controls the surgical robot through a console located in the operating room.
This technique is practiced when it is medically possible and indicated for all types of surgery, whether of the stomach, small intestine, colon, rectum, liver, pancreas or spleen in benign and oncologic indications. Robotic surgery has the advantage of magnification of the visualized image up to 10 times, provides a three-dimensional vision and offers endowristed instruments with 7 degrees of freedom.
These benefits of the robotic technology help for precise dissection and reconstruction also in spaces more difficult to access, therefore allowing the indications for minimally invasive surgery to be extended to indications that would otherwise have to be done through the open approach.
Augmented reality
Contenu
Augmented reality consists in superimposing an image artificially generated on a real-world image, in order to show what the human eye cannot see. In digestive surgery, when medically indicated, the surgeon can use a camera to visualize the blood vessels and the perfusion of the organs by a technique superimposing an image obtained by fluorescence and an image of the organs in real-time. This technique allows to check the perfusion of an organ (for example the intestine), to visualize the blood vessels or important anatomical structures, and to choose the optimal surgical strategy.
Accelerated rehabilitation
Contenu
Accelerated rehabilitation protocols (also named "fast-track" protocols) are validated protocols of therapeutic care which aim at optimizing the pre-operative and post-operative care of patients undergoing surgery in order to accelerate their recovery and reduce their risk of complications. The Division of Digestive Surgery systematically applies these protocols to offer the best possible care to patients.
Negative pressure therapy
Contenu
Negative pressure therapy involves applying a special type of wound dressing connected to a suction pump that produces vacuum on the wound. This technique aims to aspirate fluids that may be released from the wound and stimulate vascularization of the edges of the wound, helping to speed up healing and reduce the risk of infection. Negative pressure therapy can be applied on an open wound, on a closed wound, or on a cavity (such as the esophagus or rectum).
The latest development in materials engineering
Contenu
Driven by a constant determination to provide patients with the latest innovations in surgical technologies, we regularly reassess our offer in terms of surgical implants, in particular for abdominal wall surgery (hernia surgery), and offer, when medically indicated, innovative prostheses, degradable or not, synthetic or biological.
Advanced chemotherapy techniques
Contenu
Some cancer patients need chemotherapy, drugs usually given through the vein to help them to fight cancer. In advanced cancer, it may be necessary to directly administer chemotherapy into the abdominal cavity. For this purpose, the Division of Digestive Surgery offers, in medically selected cases, hyperthermic intraperitoneal chemotherapy (CHIP) et la chimiothérapie intrapéritonéale pressurisée par aérosols (PIPAC – pressurized intraperitoneal aerosol chemotherapy).

 Digestive surgery, also named visceral or abdominal surgery, is the surgery of digestive organs, such as:
Digestive surgery, also named visceral or abdominal surgery, is the surgery of digestive organs, such as: